1 yr old baby is admitted with fever 3 days cough 2 days and breathlessness one day. She was feeding well ,but today became more dyspneic and was not feeding well
No h/o chd,fb
O/e. Rr 60/Mt,spo2 90%,hr 138/Mt,
temp 102 f
Retraction lower chest,suprasternal,
Prominent sternocleidpmastoid
Grunt+
Subcostal area a dip seen
Dx: severe pneumonia
Why there is tachypnea in pneumonia?
Tachypnea, defined according to World Health Organisation (WHO) recommendations, was present in 74% of children with pneumonia and in 33% of those without pneumonia.
When there is hypoxia ,co2 accumulation stimulate the chemoreceptors ,which relay to Respiratory centre breath faster to maintain the minute volume which is tidal volume ×respiratory rate
The tidal volume is reduced in pneumonia ,so naturally respiratory rate has to be increased to.maitain minute volume
Why there is retraction?
Th e work of inspiration is the sum of the work necessary to overcome the elastic forces of the lung, the tissue viscosity of the lung and chest wall, and airway resistance.
When any of these factors is increased (eg, elastic force and tissue viscosity in restrictive pulmonary disease, resistance in obstructive airway disease), the work of inspiration must increase to maintain adequate & VE.
Th e accessory muscles of inspiration (the sternocleidomastoid, anterior serratus, and external intercostal muscles) are recruited to accomplish this task.
Contraction of these muscles causes forceful expansion of the thorax, resulting in an unusually large negative intrathoracic pressure.
Th is negative pressure draws in the soft tissues of the chest wall and creates 1 of the classic signs of dyspnea, retractions, which may be seen in the suprasternal, infrasternal, intercostal, subcostal, and supraclavicular areas.
Why there is Grunt?
Is an early closure of glottis to increase the end expiratory pressure to prevent collapse if alveoli and smaller airway
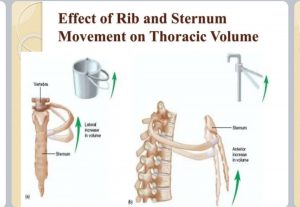
How does accessory muscles help pneumonia child?
They have bucket handle action of lifting ribs and sternum ,so they increase intrathoracic volume
Why alae nase is prominent?
There is a muscle called dilator nares ,which when contracts decreases upper airway resistance
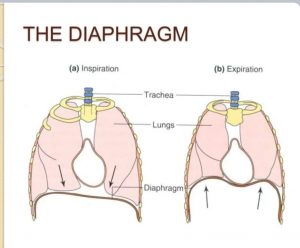
Why subcostal Retraction in pneumonia?
Diaphragm is the muscle of inspiration, but when it is contracting against resistance and faster you get subcostal Retractions
What is the treatment for severe pneumonia?
For Severe Pneumonia (Children with respiratory distress requiring indoor care)-
Under 2 months of age: o Inj Cefotaxime / Ceftriaxone and Gentamicin for 10 days
Over 2 months of age: o Inj. Ampicillin (50mg/kg/dose 6h) + Gentamicin (7.5mg/kg/day OD i.m or i.v) is used.
Inj Ampicillin can be switched to Oral Amoxycillin (45mg/kg/day TDS) once child is stable and able to take oral feeds. Total treatment duration is 7-10 days.
o In case of no response in 2 days the patient is assessed for complications like empyema, or infection at any other site.
In the absence of any complication, a 3rd generation Cephalosporin (Cefotaxime 50mg/kg/dose 6h or Ceftriaxone 75- 100mg/kg/day in two divided doses, IV ) is used and can be switched to oral Cefopodoxime (10mg/kg/day BD) once the child is able to take orally. Total treatment duration is 7-10 days.
o In case the patient has severe sepsis/ septic shock, Inj. Piperacillin + Tazobactam (90mg/kg/dose 6h) + MRSA cover with IV Vancomycin (15mg/kg/dose 6h) is recommended.
CASE 2
2 yr old treated for pneumonia for 10 days is referred because of persiti g fever and a cavity like lesion in rt mid zone
Dx staph pneumonia with pneumatocele /lung abscess
How to suspect staph pneumonia ?
Rapid progression of the disease,
or Pneumatocele, or Pneumothorax, or Effusion on chest X ray
Large skin boils or abscess or infected scabies or
Post measles pneumonia, which is not responding within 48 hours to the initial therapy
What is the implications of persisting fever Ina child with pneumonia?
The response usually occurs by 48 to 96 hrs
In case of no response in 2 days the patient is assessed for complications like empyema, or infection at any other site
This should done with chest radiography and ultrasound. Ultrasound has better sensitivity and specificity than xray
We consistantly do ultrsound for such as point of care ultrasound
what is pneumatocele ?
After pneumonia, inflammation, and narrowing of the bronchus leads to the formation of an endobronchial ball valve that leads to the distal dilatation of the bronchi and alveoli.
The obstruction is believed to be caused by inflammatory exudates within the airway lumen or wall, allowing air to enter the cystic space but not to leave it.
Subsequent enlargement of the pneumatocele occurs either due to pressure from the adjacent pneumatocele or intraluminal inflammatory exudates.
What are the complications of staph pneumonia?
Empyema, necrotising pneumonia,bronchpleural fistula,lung abscess
Spread to nearby organs ,distant spread can cause other System involvement
What isbthe role ultrasound in staph pneumonia?
[Sonographic findings of loculations and septations with in effusion shas been shown to correlate with empyema as confirmed by surgical findings and fluid analysis
A chest ultrasound of a 7 yr female which demonstrates a right sided mul-septated, moderate to large, hyperechoic pleural effusion with a thickened visceral pleural ’rind’ appearance.
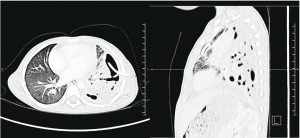
Computed tomography imaging of a 4yomale with pneumococcal pneumonia (serotype 3) complicated by left sided empyema and bronchopleural fistula.
The imaging demonstrates a left sided hydropneumothorax with consolidaon of the left upper and lower lung segments, and loss of the normal pulmonary parenchyma consistent with a necrosing pneumonia, with a flexible chest drain insitu
WHAT is treatment of empyema?
EMPYEMA
• Proper drainage : Forms the main core of treatment.
Antimicrobial Therapy: Anti- Staphylococcal penicillin (Cloxacillin 100-200 mg/kg/day) along with 3rd generation cephalosporin like Ceftriaxone may be used as first line drug.
Co-Amoxyclav is alternative first line therapy.
In seriously ill patients with disseminated staphylococcal disease and septic shock to cover for MRSA, Vancomycin is recommended. Vancomycin is less effective than the first line drugs for the commoner Methicillin sensitive strains of Staphylococcus aureus.
Children may continue to be febrile for 5-7 days after starting antibiotic therapy in the case of S. pneumoniae and H. influenzae and for 10-14 days in the case of Staphylococcus aureus. The clinical response to therapy should be assessed with parameters such decrease in fever, normalization of lab parameters such as CBC count, CRP, decrease in drain volume, clearing in chest x-ray, improvement in the overall condition of the patient.
The decline in toxicity and fever are good signs of likely response. In case of complete non response after 96 hours of treatment, high spiking fever and persistent drainage, second line treatment may be instituted. Vancomycin should be substituted instead of the first line cloxacillin or co-amoxyclav.
All children with non response should be evaluated for presence of pus pockets in the pleural cavity by an ultrasound chest. Here the key lies in better drainage rather than in a change of antibiotics. Extraneous causes of fever should also be evaluated.
CASE 3
24yr old has fever 3 days cold 2 days ,sorethroat and malaise. He was tested for coivid which was negative.at home parents have sim8lar illness.he is now breathlessness with rr 59 /mT
What could be the dx?
Ili
H1n1 pneumonia
How to distinguish viral pneumonia from bacterial pneumonia?
Bacterial –
is considered abrupt in onset, with the febrile patient appearing ill and sometimes toxic.
Respiratory distress is moderate to severe; auscultatory findings may be few and focal, limited to the involved anatomic segment.
Signs and symptoms of sepsis and localized chest pain (signifying pleural irritation) are more suggestive of bacterial etiology [10], as they are rarely present in nonbacterial pneumonia.
Complications, like lungvabscess,empyema ,necrotising pneumonia are more suggestive of bacterial etiology () On the other hand, typical bacterial pneumonia is unlikely in children older than five years if wheezing is present [23]. Pneumococcal pneumonia is the most common typical bacterial pneumonia in children of all ages. Fever and cough occur in the majority of children with pneumococcal pneumonia. Other common findings include malaise/lethargy, decreased breath sounds, and crackles.
Viral
Viral – The onset of viral pneumonia is gradual and associated with preceding upper respiratory tract symptoms (eg, rhinorrhea, congestion). The child does not appear toxic. Auscultatory findings are usually diffuse and bilateral.
In one study of 98 ambulatory children with pneumonia, wheezing was more frequent in patients with viral than bacterial pneumonia (43 versus 16 percent), but other clinical features often associated with viral illness, such as rhinorrhea, myalgia, and ill contacts, were not [26].
Some viral causes of pneumonia are associated with characteristic dermatologic findings: • • Measles , Varicella
Whatbis the treatment for hini?
Case definition of ILI ( Influenza Like Illness )
An acute respiratory infection with:- • Measured fever of ≥ 38 C° (≥100oF) • And any of the respiratory symptoms including coryza, sore throat, cough with onset within the last 10 days.
CASE 4
6 yr old boy has low grade fever ,nonprooductive cough snice 5 days .he was on amoxycillin with no improvement. He has body ache, headache and conjunctivitis
Is he a candidate for mycoplasma pneumonia?
– “Atypical” bacterial pneumonia resulting from Mycoplasma pneumoniae or Chlamydia pneumoniae usually presents abruptly with constitutional findings of fever, malaise and myalgia; headache; photophobia; sore throat; conjunctivitis; rash; and gradually worsening nonproductive cough despite improvement of other symptoms [19,23].
Although hoarseness may be seen in disease caused by both agents, it s more frequently seen with C. pneumoniae infection.
Wheezing is a frequent finding in atypical bacterial and viral pneumonias
What is the treatment?
Classically the mycoplasma pneumonia presents in an atypical fashion but literature suggests that it can sometimes be difficult to distinguish mycoplasma pneumonia from a pyogenic pneumonia.
Macrolide antibiotics should be considered in following clinical scenarios where the likelihood of mycoplasma pneumonia is high:
a. Children with a subacute presentation with prolonged low grade fever, persistent cough, chest signs out of proportion to the radiographic abnormality (usually showing perihilar streaky infiltrates).
b. Children with CAP (acute pneumonia like presentation with radiological evidence of patchy or lobar consolidation) who also have or develop extrapulmonary manifestations like myocarditis, hemolytic anemias, glomeruonephritis, aseptic arthritis, CNS problems (aseptic meningitis, encephalitis, ataxia), etc.
c. Non response to first line antibiotics in children who are immunized with Hib/PCV and have no suppurative complications of CAP.
How do you treat necrotising pneumonia and lung abscess?
Suspect necrotising pneumonia when there is hypolucent lesion in an area of consolidation
Necrotizing pneumonia, necrosis, and liquefaction of lung parenchyma is a serious complication of CAP. Necrotizing pneumonia usually follows pneumonia caused by particularly virulent bacteria [121]. S. pneumoniae (especially serotype 3 and serogroup 19) is the most common cause of necrotizing pneumonia [122-125].
Necrotizing pneumonia also may occur with S. aureus and group A Streptococcus and has been reported due to M. pneumoniae, Legionella, and Aspergillus [12. linical manifestations of necrotizing pneumonia are similar to those of uncomplicated pneumonia, but they are more severe [130-132]. Necrotizing pneumonia should be considered in a child with prolonged fever or septic appearance [121].
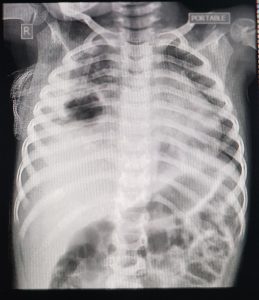
The diagnosis can be confirmed by Doppler ultrasonography, chest radiograph (which demonstrates a radiolucent lesion) ( image 1), or contrast-enhanced computed tomography (CT) ( image 3) if the diagnosis remains uncertain [133,134].
The findings on chest radiograph may lag behind those of CT and Doppler ultrasonography may detect necrotic changes earlier than CT [1
Lung abscess —
A lung abscess is an accumulation of inflammatory cells, accompanied by tissue destruction or necrosis that produces one or more cavities in the lung [40]. Abscess formation may result from inadequate or delayed treatment of lobar pneumonia or more commonly develops one to two weeks following an aspiration event.
Other predisposing factors include airway obstruction and congenitally abnormal lung [40]. Anaerobic flora of the upper respiratory tract and S. aureus are the organisms most frequently involved
Clinical manifestations of lung abscess are nonspecific and similar to those of pneumonia [40]. They include fever, cough, dyspnea, chest pain, anorexia, hemoptysis, and putrid breath [121,136-138]. The course may be indolent.
The diagnosis is suggested by a chest radiograph demonstrating a thick-walled cavity with an air-fluid level ( image 1) [40] and confirmed by contrast-enhanced CT in questionable clinical situations or if necessary before invasive interventions (eg, percutaneous aspiration, placement of a drainage catheter) [133]. Lung abscess is often accompanied by parapneumonic effusion [139,140].
Lung abscess should be suspected when consolidation is unusually persistent, when pneumonia remains persistently round or mass-like, and when the volume of the involved lobe is increased (as suggested by a bulging fissure
CASE 5
5 yr old child with asd is in contact covid positive mother.he develops fever sorethroat after 5 days . He has breathing difficulty for the last two days. He is now covid positive and has rt lower zone haziness. Usg shows halo like peripheral lesion in lower lobe
Aby ph 7.2,pci2 48mmhg,pao2 58mm hg
How do you treat?
Severe acute COVID-19, which is SARS-CoV-2 infection with 1 or more organ system involvement
Detection of SARS-CoV-2 nucleic acid using real-time reverse transcriptase polymerasechainreaction (RT-PCR)is considered the gold-standard for thediagnosis of COVID-19.21 The virus can be detected in the upper airway (nasopharynx swab) or lower airway secretions (tracheal aspirates, bronchoalveolar lavage), blood, urine, and stool.
Leukocytosis or leukopenia, lymphocytosis or lymphopenia, and increases of CRP, serum ferritin, lactate dehydrogenase (LDH), D-dimers, procalcitonin, erythrocyte sedimentation rate (ESR), serum aminotransferases, and creatine kinase myocardial bands (CK-MB) have been observed.22,23
Increases of CRP, procalcitonin, pro–B-type natriuretic peptide (BNP) and platelet count are more common in children
Hyperinflammation associated with increased LDH, D-dimer, IL-6, CRP, and ferritin, and decreased lymphocyte count, platelet count, and albumin level were associated with worse outcomes in adult patients with COVID-19.
Although chest radiographs do not have high sensitivity and specificity for the diagnosis of COVID-19, they are useful to monitor disease progression. Bilateral distribution with presence of peripheral or subpleural ground-glass opacifications and consolidation are common findings in COVID-19 pneumonia or ARDS
Typical features of viral respiratory infections in children, such as increased perihilar markings and hyperinflation, were not reported in children with COVID-19.27
Computed tomography (CT) scans are considered the gold standard for imaging with COVID-19 respiratory disease.29 CT scans are highly sensitive and specific and can detect infection before the appearance of clinical signs.29,30
Three phases of evolution have been observed in children with COVID-19 disease
. These phases are the halo sign, defined as nodules or masses surrounded by ground-glass opacifications seen in the early phase of the disease;
widespread ground-glass opacifications in the progressive phase; and
consolidative opacities in the developed phase. Peribronchial thickening and inflammation along the bronchovascular bundle are observed more frequently in children than adults.31 Fine mesh reticulations and so-called crazy-paving sign have been reported. Pleural effusion and lymphadenopathy are rare.31
chest CT is not recommended as the initial diagnostic test in children suspected of having COVID-19. However, it may be considered to answer specific clinical questions such as presence of pulmonary embolism, for assessment of those not responding to treatment,and to track evolution of fibrotic disease.
Lung ultrasonography is a useful imaging modality because semiquantitative scores in lung ultrasonography have been shown to be consistent with those in lung CT scans in adults who are critically ill with COVID-19, and should be considered in children
Antiviral therapy: remdesivir is an antiviral medication that is an inhibitor of the SARS-CoV-2 RNA-dependent RNA polymerase (RdRp), which is essential for viral replication.
Remdesivir is approved by the US Food and Drug Administration (FDA) for treatment of patients greater than or equal to 12 year old hospitalized with COVID-19 who weigh greater than or equal to 40 kg, and is FDA authorized via EUA for use in hospitalized patients less than 12 years of age or weighing from 3.5 to less than 40 kg.42,4
Children weighing greater than or equal to 3.5 kg and less than 40 kg should receive a loading dose of 5mg/kgonday1followedby2.5mg/kg/doseoncedaily.Forthose greater than or equal to 40 kg, a loading dose of 200 mg is recommended on day 1 followed by 100 mg daily.
Duration of therapy is 5 days or until hospital discharge, whichever is earlier, and 10 days for those who require mechanical ventilation or ECMO.
6 months old child with a weight of 4.5 kg is admitted with severe pneumonia.mother is also to have pneumonia and recurrent infection.baby has oral thrush and is partially immunized. We havevstarted ampicillin and gentamicin but baby has fever on day3,but no complications. Wr switched to ceftriaxone ,now it is day 6 but running fever sat of 90%
What should be our considerations?
Pneumocystis jiroveci Pneumonia should be suspected in any HIV-positive infant with severe pneumonia.(pneumonia +oral thrush+sick mother) If PCP is untreated, mortality from this condition is very high. It is therefore imperative to provide treatment as early as possible.
Diagnosis ■ is most likely in a child < 12 months (peak age, 4–6 months),
■ subacute or acute onset of non-productive cough and diffi culty in breathing,
■ no or low-grade fever,
■ cyanosis or persistent hypoxia,
■ poor response to 48 h of fi rst-line antibiotics for pneumonia, and
Treatment
Promptly give oral or preferably IV high-dose co-trimoxazole (8 mg/kg trimethoprim–40 mg/kg sulfamethoxazole) three times a day for 3 weeks.
If the child has a severe drug reaction, change to pentamidine (4 mg/kg once a day) by IV infusion for 3 weeks.
Prednisolone at 1–2 mg/kg per day
Prednisone doses (beginning as early as possible and within 72 hours of PCP therapy): Days 1–5: 40 mg orally twice daily; 1 mg/kg/dose twice daily (children) Days 6–10: 40 mg orally daily; 1 mg/kg/dose once daily (children) Days 11–21: 20 mg orally daily; 0.5 mg/kg/dose once daily (children)
may be helpful early in the disease if severe hypoxia or severe respiratory distress is present.
Continue co-trimoxazole prophylaxis on recovery, and ensure that ART is given.
■ elevated levels of lactate dehydrogen
Laboratory monitoring during remdesivir therapy should include CBC, CMP, PT/International Normalized Ratio (INR) at baseline, day 5 of therapy, and moreoften if there is concern for toxicity. C
How to treat a child with spastic quadriplegia and h/o aspiration ?
Aspiration pneumonia — Empiric antibiotic regimens for community-acquired aspiration pneumonia must cover oral anaerobes. Appropriate antibiotic regimens for hospitalized children include [67]:
● ● Ampicillin-sulbactam 150 to 200 mg/kg per day of the ampicillin component IV in four divided doses; maximum 8 g/day of the ampicillin component,
or Clindamycin 30 to 40 mg/kg per day IV in three or four divided doses to a maximum of 2.7 g/day if MRSA etiology is suspected or for patients unable to receive beta-lactam antibiotics (eg, history of IgE-mediated reaction or severe delayed hypersensitivity reaction
Appropriate antibiotic regimens for children with health care-associated aspiration who are known to be colonized with unusual gram-negative pathogens (eg, Klebsiella pneumoniae) include:
● Piperacillin-tazobactam 300 mg/kg per day IV in four divided doses up to a maximum of 12 g/day, or Meropenem 60 mg/kg per day IV in three divided doses, up to a maximum of 6 g/day.
Vancomycin should be added to the empiric regimen if MRSA is a consideration. Meropenem may be preferred for gram-negative coverage if vancomycin is added because the combination of vancomycin and piperacillin-tazobactam has been associated with increased risk of acute kidney injury [73,74].
Ceftaroline is an alternative to vancomycin if MRSA is a consideration.
How to treat pneumonia in a child with febrile Neutropena?
Neutropenia alone does not appear to predispose to either viral or Pneumocystis pneumonia (PCP
Neutropenia increased incidence of Pseudomonas aeruginosa Stenotrophomonas spp. Burkholderia spp.and Other opportunistic bacteria.vruses like Aspergillus spp. Pseudallescheria boydii Agents of mucormycosis may cause infection
How to treat a child admitted for gbs developing pneumonian on ventilator on day five?
Pseudomonas or Klebsiella pneumonae Or Acinetobacter species may be the gram positive bacteria and staph aureus the gram positive one
Piperacillin tazo bacterial plus aminoglycoside or antipseudomonas fluroquinolone ( levofloxacin)may be the first choice
Vancomycin or line,old may be choice for staph
2nd choice merpenam plus vancomycin







 Superintendent, ICH.
Superintendent, ICH.