1 yr old child with h/o delayed mile stone in gross motor and adaptive domains has abnormal movements of both upper and lower limbs
High bp from 6th month antenatal
H/o perinatal depression
Seizure on day7
Hypoglycemia on day 8
Now the child has
Microcephaly, head control+,not sitting with support,does not turn over
No abnormal posture
No atnr
No parachute
No scissoring
Stiffening limbs on ventral suspension
Reflexes Exaggerated
Spasticity b/l
No Contracture
No squint
Vision follows objects
One word amma
Provisional dx :
Cerebral palsy
Spastic b/l
How to diagnose cp in infants?
For infants ≤5 months corrected age, the most predictive tools for detecting risk for CP are termage magnetic resonance imaging (MRI) (86–89% sensitivity), the Prechtl Qualitative Assessment of General Movements (98% sensitivity), and the Hammersmith Infant Neurological Examination (90% sensitivity)
For infants ≥6 months corrected age, the most predictive tools for detecting CP risk are MRI (86–89% sensitivity), the Hammersmith Infant Neurological Examination (90% sensitivity), and the Developmental Assessment of Young Children (83% C index) (8).
What are the early signs of cp?
In a baby 3 to 6 months of age:
Head falls back when picked up while lying on back
Feels stiff
Feels floppy
Seems to overextend back and neck when cradled in someone’s arms
Legs get stiff and cross or scissor when picked up
In a baby older than 6 months of age:
Doesn’t roll over in either direction
Cannot bring hands together
Has difficulty bringing hands to mouth
Reaches out with only one hand while keeping the other fisted
In a baby older than 10 months of age:
Crawls in a lopsided manner, pushing off with one hand and leg while dragging the opposite hand and leg
Scoots around on buttocks or hops on knees, but does not crawl on all fours
What are the functional classification?
The Gross Motor Function Classification System (GMFCS) is used to describe gross motor function, especially the ability to walk, for children from 2 to 18 years of age (19,20).
GMFCS is used to describe self-initiated movements as well as movements assisted by devices such as walkers, crutches, canes or wheelchairs (19,20).
The Manual Ability Classification System (MACS) is used to describe the typical use of both hands and upper extremities for children from 4 to 18 years of age (21).
The Communication Function Classification System (CFCS) is used to describe the ability of persons with CP for daily routine communication (sending or receiving a message) (22). The CFCS considers all methods of communication including vocalizations, manual signs, eye gaze, pictures, communication boards or speech generating devices (22).
The Eating and Drinking Ability Classification System (EDACS) is used to describe the eating and drinking function for children 3 years and older (23). The EDACS assesses the eating and drinking safety (risk for aspiration or chocking), and eating and drinking efficiency (the amount food lost and the time taken to eat)
What is general movement?
Writhing Movements
During term age and during the first 2months post-term,GMscommonly are referred to as writhing movements.They are characterized by small to-moderate amplitude and by slow-to moderate speed.Typically,theyare elliptical inform,which createsthe impression of a writhing quality[Hopkins andPrechtl,1984;PrechtlandHopkins, 1986;Cionietal.,1989;Prechtletal., 1997a,1997b].EMG recordings revealed thatcthe burstcduration was significantly longer during preterm GMs than during writhingmovements.However,burst amplitude values and tonic background data do not change from preterm GMs to writhing GMs
[Hadders- AlgraandPrechtl,1993].
FidgetyMovements
At 6 to 9weekspost-termage, writhing movementsc gradually disappear whereas fidgetyGMs gradually emerge [HopkinsandPrechtl,1984;Cioniand Prechtl,1990;Hadders-Algraand Prechtl,1992;Prechtletal.,1997b].
Fidgety movements are of small amplitude,moderate speed,and variable acceleration of neck,trunk,and limbs in all directions continually in the awake infant except during fussing and crying
What are the MRI findings suggestive of cp?
The most predictive patternsare
(1)white matter injury (cystic periventricular leukomalacia or periventricular hemorrhagicinfarctions) (56%),
(2)cortical and deep gray matter lesions(basalganglia or thalamus lesions,watershed injury[parasagittal injury],multicysticencephalomalacia,orstroke)(18%),and
(3)brain maldevelopments (lissencephaly,pachygyria,corticaldysplasia, polymicrogyria, or schizencephaly
what is cp?
Cerebral palsy (CP) describes a group of permanent disorders of the development of movement and posture, causing activity limitation, that are attributed to nonprogressive disturbances that occurred in the developing fetal or infant brain. The motor disorders of cerebral palsy are often accompanied by disturbances of sensation, perception, cognition, communication, and behaviour, by epilepsy, and by secondary musculoskeletal problems.
What are the components of cp Classification?
Components of CP classification
1. Motor abnormalities
A. NATURE AND TYPOLOGY OF THE MOTOR DISORDER: The observed tonal abnormalities assessed on examination (e.g. hypertonia, hypotonia) as well as the diagnosed movement disorders present, such as spasticity, ataxia, dystonia, athetosis.
B. FUNCTIONAL MOTOR ABILITIES: The extent to which the individual is limited in his or her motor function, including oromotor and speech function
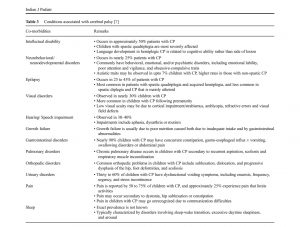
. 2. Accompanying impairments The presence or absence of later-developing musculoskeletal problems and/or accompanying non-motor neurodevelopmental or sensory problems, such as seizures, hearing or vision impairments, or attentional, behavioral, communicative and/or cognitive deficits, and the extent to which impairments interact in individuals with cerebral palsy.
3. Anatomical and neuro-imaging findings
A. ANATOMIC DISTRIBUTION: The parts of the body (limbs, trunk, bulbar region, etc.) affected by motor impairments or limitations. B. NEURO-IMAGING FINDINGS: The neuroanatomic findings on CT or MRI imaging, such as ventricular enlargement, white matter loss or brain anomaly.
4. Causation and timing
Whether there is a clearly identified cause, as is usually the case with post-natal CP (e.g. meningitis, head injury) or when brain malformations are present, and the presumed time frame during which the injury occurred, if known.
What are the clinical 4nfeatures?
What are the associated problems?
What are the investigation?
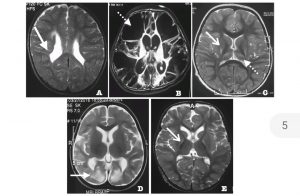
Salient MRI changes in cerebral palsy.
Panel A shows a T2 weighted image with periventricular hyperintensities and undulating ventricular margins (solid arrow). This is typically seen in prematurity associated insult and commonly manifests as spastic diplegia.
Panel B shows multi cystic encephalomalacia (dotted line with arrow). This pattern of watershed lesions is seen commonly in term infants with ischemia/ asphyxia and manifests clinically with spastic quadriplegia.
Panel C illustrates T2 hyper intensities in posterior putamen (open arrow) and thalami bilaterally (dotted line with closed arrow). This is typically seen in infants with term hypoxic ischemic encephalopathy (HIE) and manifests as dyskinetic cerebral palsy.
Panel D highlights T2 hyper intensities in occipital lobe (solid arrow); characteristic of neonatal hypoglycemic insult. Panel E shows T2 hyper intensity involving bilateral globuspallidi (open arrow), a feature of kernicterus sequelae
What is the role of physiotherapy?
Physical therapy (PT) is an integral part of CP management and may range from a regular exercise program to variety of modalities including electrical stimulation.
PT aids in encouraging caretakers to learn how best to handle, toilet, wash, and feed their children with CP and to promote posture, mobility, and transfer.
What is the role of occupational therapy?
Occupational therapy (OT) techniques seek to improve function, but focus on maximizing a child’s ability to accomplish activities of daily living, education, and work. These are particularly helpful in maximizing available hand function.
Which all ot and pt methods are recommended?
The PT and OT based approaches which have been recommended in literature include [9]:
1. Bimanual training for hemiplegic CP where the child is trained to use bothhands togetherthrough repetitivetasks.
2. Constraint induced movement therapy involves restraint of the unaffected limb to encourage the use of affected limb during the therapeutic tasks. The restraint may be by the use of casting or physically restraining by holding the normal hand.
3. Context focused therapy involves changing the environment rather than the child’s approach.
4. Goaldirected functional training lays emphasis on activities based on goals set by the child, using motor learning approach.
how to manage spasticity?
Management of Spasticity
Tone reduction may be considered if hypertonia or spasticity interferes with function, comfort, or care. But before venturing for tone reduction, it should be confirmed that the “increased tone” is not beneficial to the child; for example, some patients with severe lower extremity hypertonia use their heightened tone to “stand up” onotherwise weaklimbsand maylosetheir ability to stand and bear weight through their legs after treatment. Hence a team approach with pre-decided goals is essential.
Which all are the oral medications?
Oral antispasticity agents including benzodiazepines, baclofen and tizanidine have the advantage of ease of administration but the disadvantages of systemic effect and significant sideeffects [10, 11]. Thus, they are most appropriate for children with generalized spasticity, and/or in children in whom only mild tone reduction is needed. Unfortunately, the evidence on the efficacy of these agents is less rigorous. Hence, the choice of the agent ismoreamatterofpersonalexperiencerather than evidence-based medicine
Baclofen
Bind to GABAB receptors of laminae I − IV of the spinal cord, where primary sensory fibers end, thereby inhibiting the release of excitatory neurotransmitters and causing presynaptic inhibition of mono- and polysynaptic reflexes
Initial doses, titrated to effect (review treatment if no benefit within 6 wk):
• 1–6y:0.3mg/kg/din3–4 divided doses, increased to 0.75–2 mg/kg/d (or 10–30 mg/d) in 3–4 divided doses
• 6–8y:0.3mg/kg/din3–4 divided doses, increased to 0.75–2 mg/kg/d (or 30–40 mg/d) in 3–4 divided doses
• 8–10 y: 0.3 mg/kg/d in four divided doses, increased to 0.75–2 mg/kg/d (or 60 mg/d) in 3–4 divided doses
• 10–18 y: initially 5 mg three times daily increased gradually, up to 60 mg/d (max. 100 mg/d
Tizanidine
Acts as a central α-2 receptor agonist at supraspinal and spinal levels to reduce spasticity by inhibition of spinal polysynaptic reflex activity.
Initial dose < 10 y: 1 mg twice daily >10y:2mgOD • Maximum 0.05 mg/kg/d >12y:2mgTDS
Diazepam
Acts post-synaptically by binding toaspecificsiteof the gamma-aminobutyric acid A receptor (GABAA), enhancing the endogenous effects of GABA as an inhibitory neuro-transmitter
Initial doses titrated to effect:
• 1–12 mo: 0.25 mg/kg twice daily • 1–5 y: 2.5 mg twice daily
• 5–12 y: 5 mg twice daily
• 12–18 y: 10 mg twice daily (maximum 40 mg/d)
What is the role inj botox?
Botulinum toxin type A (BTX-A) when injected into the affected muscles, blocks the presynaptic release of acetylcholine from motor endplates of the lower motor neuron and decreases tone by limiting muscle contraction. Hence it produces chemodenervation.
The best evidence for use of BTX-A is for equines varus (treated by injections into the gastrocnemiussoleus muscles), but BTX-A is now used for a variety of focal indications including knee and hip flexion spasticity, and spasticity of the upper extremity.
Patients younger than 4 y old and without fixed contractures are expected to have the most favorable able response because the musculoskeletal and nervous system is most plastic in growing children [12].
Nonetheless, BTX-A also may be useful to treat focal dystonias in older children and adults.
The total dosage ceiling used by experienced injectors has risen from the initial recommendation of 4 U/kg to greater than 16 U/kg in specific specialist cases; but the dosing has to be individualized
Phenol and Alcohol
Phenol and alcohol are the other agents associated with chemodenervation, and have been used in children with CP, although neither has been rigorously tested. Phenol is typically injected at a concentration of 3%–6% aqueous solution, whereas absolute alcohol is diluted to 30%–50%. The target nerve is identified with electrical stimulation, a procedure that may be poorly tolerated in children, making sedation or anesthesia necessary. The agent is injected perineurally, where it promotes denervation via axonal degeneration
Intrathecal Baclofen
Intrathecal baclofen (ITB), administered via acatheterattached to a programmable pump implanted subcutaneously, achieves higher cerebrospinal fluid drug levels as compared with oral administration, but may also be associated with substantial complications.
What are the surgical therapies?
Surgical Therapy Selective Dorsal Rhizotomy (SDR)
SDR is asurgical procedure that selectively divides parts of the dorsal lumbosacral roots of the spinal cord. This interrupts the afferent limb of the reflex arc on the sensory side, thus reducing spasticity without causing paralysis. This technique may provide a small gain in function.
Candidates for SDR are typically ambulatory or nearly ambulatory (GMFCS levels II and III, sometimesGMFCSlevelI),arebetween4and7yofage, have spared cognitive skills and are motivated to walk, have some degree of preserved selective motor control in the lower extremities, have adequate strength, and have minimal, if any, dystonia. In addition, the family must be able to commit to a rigorous daily physical therapy program for 6 to 12 mo [13].
Deep Brain Stimulation
Deep brain stimulation (DBS) is primarily used for dystonias. Ameta-analysis of DBS in adults with dyskinetic CP suggests that it may be effective [14]
How do you treat dystonia?
Trihexyphenydyl
Anticholinergic agent works at the level of the basal ganglia
Start with initial low dose (1–2 mg/d); increase slowly (by 2 mg/wk); higher doses (>50 mg/d) might be needed • Usual dose: 2–60 mg/d in 2–3 divided doses
Initial dose: 12.5 mg/d • Titrate to maximum dose 150 mg/d in 2 divided doses
Tetrabenazine
Dopamine depletors, prevent neurotransmitter degradation
When to do orthopedic Interventions?
Orthopedic Interventions
Timing of surgery depends on CNS maturation, ambulation potential, and rate of deformity development.
The nervous system matures around the age of 4 to 6 years when the physician can assess muscle imbalance more accurately; predict a functional prognosis; and make sure that no other abnormalities, such as athetosis or dystonia, are present.
Therefore, soft tissue procedures are generally performed between 4 and 7 years of age,
hand surgery between 6 and 12 years of age, and
bony procedures after 8 years of age although it is the needs of the child that determine the exact timing.
Exceptions are progressive hip instability and deformities and contractures interfering with function.18,
Dr jp ich ktm
What is the role of assitive devices?
Assistive Devices
A child who has CP needs to move around, to explore his or her surroundings, and to interact with his or her peers so that his or her mental, social, and psychologic skills develop to the fullest.
A variety of mobility aids and wheelchairs provide differing degrees of mobility to these children.
Transfer aids, such as lift systems, assist the caregiver when performing transfers.
Passive standing devices called standers allow the child to get accustomed to standing erect and provide therapeutic standing.
Some ambulatory children use gait aids, such as walkers, crutches, and canes, in addition to braces for efficient and safe ambulation.
Gait aids mainly used to improve balance also decrease energy expenditure, decrease the loads on the joints, and improve posture and pain. Nonambulatory children use wheelchairs for moving around. Wheelchairs must be properly fitted with seating aids, cushions, and other positioning components.
What is role advanced technology?
Advanced technology
Augmentation technology where finger movements can drive the wheelchair ; ; ;
Substitution technologies including speech technology ; ;
Robotic-assisted gait trainers (RAGT) and robotic ankle training (RAT) can improve the gait and Gross Motor Function Classification System (GMFCS) in children with cerebral palsy ; ; ;
Virtual reality including video games can be useful for motivating full body movement and has been found useful in balance problems and sensory perception problems
Inertial navigation system to aid mobility that senses the motion of the subject
Dr jp ich ktm
What is the role of treadmil training?
Treadmill training Treadmill training as an intervention for children with CP aims at improving balance as well as lower extremity symmetry (10,30,31,35,43-46). It provides important measures in developing an understanding of how to walk independently.







 Superintendent, ICH.
Superintendent, ICH.