How to diagnose congenital hypothyroidism?
Diagnosis. Over 95% of newborns with CH are asymptomatic at birth, but universal newborn screening permits early diagnosis and treatment, resulting in optimal neurodevelopmental outcome
What are the Indian screening guidelines?
The Indian Society for Pediatric and Adolescent Endocrinology has formulated locally relevant Clinical Practice Guidelines for newborn screening, diagnosis and management of primary congenital hypothyroidism (CH). Recommendations:
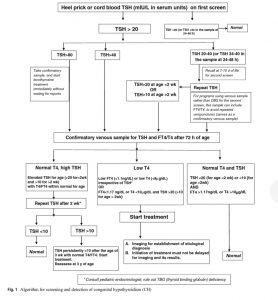
Screening should be done for every newborn using cord blood, or postnatal blood, ideally at 48 to 72 h of age.
On this screen sample, neonates with TSH>20mIU/L serum units (or >34 mIU/L for samples taken between 24 to 48h ofage)should be recalled for confirmation.For screen TSH>40 mIU/L, immediate confirmatory venous T4/FT4 and TSH, and for milder elevation of screen TSH, a second screening TSH at 7 to 10 d of age, should be taken.
Preterm and low birth weight infants should undergo screening at 48–72 h postnatalage.Sick babies should be screened at least by 7d of age.
Venous confirmatoryTSH>20mIU/L beforeage 2wk and>10 mIU/L after age 2 wk, with low T4 (<10 μg/dL) or FT4 (<1.17 ng/dL
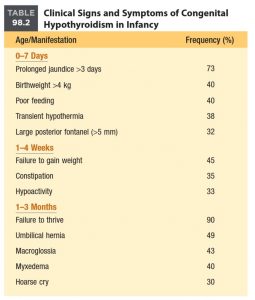
What are the clinical features?
If clinical signs of hypothyroidism are present (e.g., constipation, hypothermia, poor tone, mottled skin, prolonged jaundice, poor feeding, large tongue, open posterior fontanel), thyroid function tests should be sent immediately, even if the initial screen was normal.
Rarely, screening programs miss cases of CH as a result of early discharge, improper or no specimen colection (e.g., hospital transfers, home births, sick or premature neonates), laboratory error, delayed TSH elevation, or human error in reporting results. Primary TSH screening programs may miss infants with central (pituitary) hypothyroidism. Acquired hypothyroidism (e.g., due to postnatal excess iodine exposure) wi l also be missed on newborn screening.
.how to diagnose congenital hypothyroidism?
How to treat congenital hypothyroidism?





 Superintendent, ICH.
Superintendent, ICH.