What is bilious vomiting?
Bile is produced in the liver and stored in the gall bladder, where it appears as a golden-yellow colour. It drains via the common bile duct through the ampulla of Vater in the proximal duodenum, aiding in the digestion of lipids.
Luminal obstruction distal to the ampulla is pathological and results in the reflux of bile to the stomach, where contact with gastric acid gives it its characteristic green colour.
What is our concept?
Classical teaching dictates that bilious vomiting is due to a surgical pathology until proven otherwise e and indeed, between 20 and 50% of neonates presenting with bilious emesis will have a surgical cause.
What are the likely causes?
Broadly, bilious emesis can be due to medical or surgical causes (Figure 1). Surgical bilious emesis is almost invariably due to intestinal obstruction, however the classic triad of intestinal obstruction e bilious vomits, abdominal distension and absolute constipation (or failure to pass meconium in the neonate) e may not always be obvious in this age group.
An important distinction needs to be made between upper/proximal versus lower/distal obstruction, as management will vary quite significantly between the two
Medical
Sepsis,nec,gerd,hypothermia, chd
Surgical
Proximal
Malrotation Duplication cyst,atresia
Distal
Arm,hirschsprungs meconium ileum atresia,small left colon
What are the points in history?
History Clinical history and examination will often suggest a diagnosis, and in some cases may even obviate the need for further investigation .
Antenatal history may aid diagnosis e polyhydramnios is usually present in cases of proximal intestinal obstruction, whereas oligohydramnios may suggest distal obstruction and/or associated genitourinary abnormalities.
Gestational diabetes is associated with small left colon syndrome and can present with the appearance of distal intestinal obstruction.
Immediate post-natal history will also provide clues, in particular failure to pass meconium within 24 hours of birth and progressive abdominal distension.
Maternal risk factors for sepsis and family history should be specifically asked for.
What all.points to note in physical examination?
A distended abdomen is indicative of distal obstruction whilst proximal obstruction will range from epigastric fullness, to a flat or even sunken (scaphoid) abdomen.
Changes to the colour of the abdominal wall and umbilicus, as well as palpable bowel loops, should also be checked for.
Examination of the external genitalia and hernial orifices may demonstrate incarcerated inguinal hernias, and the anus should be checked for position and size.
In the case of a neonate with signs suggestive of distal obstruction, a rectal washout may be both diagnostic and therapeutic.
What is the role of imaging?
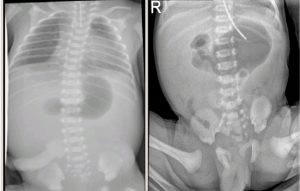
Imaging First line imaging is usually in the form of plain chest and abdominal radiograph. For a radiograph to be diagnostic, sufficient time needs to have elapsed from birth to allow for the passage of air into the abdominal viscera, usually 12 to 24 hours
Proximal obstructions may appear relatively gasless apart from the stomach region, and the classical “double-bubble” sign may be present, suggestive of duodenal atresia if no distal gas is present; however, a double-bubble appearance with distal gas is concerning for malrotation/volvulus
Providing enough time has passed to allow swallowed air to pass through the intestine, distal intestinal obstruction typically demonstrates dilated bowel loops throughout the abdomen with a paucity of gas in the rectum. Gas in the groin region may suggest inguinal hernias.
In severe cases, pneumoperitoneum may also be evident, either on standard AP radiographs or lateral decubitus
What is the role of contrast studies?
Following clinical evaluation and initial radiographic investigations, if the diagnosis remains uncertain a contrast study is usually indicated.
Upper gastrointestinal contrast (UGIC) remains the gold standard for diagnosis of malrotation/volvulus, while a lower gastrointestinal contrast enema (LGIC) may be both diagnostic and therapeutic for distal causes of obstruction.
There remains some controversy as to the optimal order of contrast studies in neonates presenting with bilious vomiting and apparent distal obstruction.
Learning point
In summary, bilious emesis in a neonate may suggest an underlying surgical pathology.
It is critical to accurately and expediently diagnose and treat malrotation/volvulus; though a relatively rare pathology only accounting for a small proportion of infants with bilious vomiting, it is time-critical and lifethreatening.




 Superintendent, ICH.
Superintendent, ICH.