7 yr old presents with cola colored urine of 2days ,puffiness of face 1 day and decreased quantity of urine
She had sorethroat 2 was ago.he is doing otherwise well
Pedal edema b/l
Bp 130/80
Puffiness of face
Healed pyoderma scars
Dx PSAGN
Why you say acute nephritis syndrome?
Hematuria(cola colored)
Generalised edema
Hypertension
How do you define hematuria?
Hematuria, defined as the persistent presence of more than 5 red blood cells (RBCs)/high power field (HPF) in uncentrifuged urine
What are the causes of hematuria?
Glomerular
1. PIGN/ IRGN 2. Ig AN 3. MPGN 4. HSP Nephritis 5. LN 6. Alport’s syndrome 7. Nail Patella syndrome 8. Thin basement membrane disease 9. Good Pasture’s syndrome
Non glomerular
1. Renal calculi 2. Renal vein thrombosis 3. Arteriovenous fistulas 4. Wilm’s tumor 5. Hypercalciuria 6. Drugs: NSAIDs, Cyclophosphamide, anticoagulants 7. Cystitis 8. Trauma
How to distinguish glomerular hematuria from nonglomerular hematuria?
Glomerular
Cola colored
Rbc cast
Proteinuria 2+
Dysmorphic rbc >30%
Acanthocytes >5%
Non glomerular
Fresh blood/
clots/
Proteinuria <2+
Dysmorpic rbc<30%
What is the aetiology of PSAGN?
APSGN follows infection of the throat or skin by certain nephritogenic strains of group A β-hemolytic streptococci.
nephritis have been described in association with throat (serotypes M1, M4, M25, and some strains of M12) and skin (serotype M49) infections, this disease is most commonly sporadic.
WHAT IS THE PATHOLOGY?
Glomeruli appear enlarged and relatively bloodless and show a diffuse mesangial cell proliferation, with an increase in mesangial matrix . Polymorphonuclear leukocyte infiltration is common in glomeruli during the early stage of the diseas
Immunofluorescence microscopy reveals a pattern of “lumpy-bumpy” deposits of immunoglobulin and complement on the glomerular basement membrane and in the mesangium.
On electron microscopy, electron-dense deposits, or “humps,” are observed on the epithelial side of the glomerular basement membrane
What is the pathogenesis?
Molecular mimicry whereby circulating antibodies elicited by streptococcal antigens react with normal glomerular antigens, in situ immune complex formation of antistreptococcal antibodies with glomerular deposited antigen, and complement activation by directly deposited streptococcal antigens continue to be considered as probable mechanisms of immunologic injury.
The search for the precise nephritogenic antigen(s) that cause disease suggests that streptococcal pyogenic exotoxin (SPE) B and nephritis-associated streptococcal plasmin receptor are promising candidates.
What are the clinical manifestations?
Poststreptococcal GN is most common in children ages 5-12 yr and uncommon before the age of 3 yr. The typical patient develops an acute nephritic syndrome 1-2 wk after an antecedent streptococcal pharyngitis or 3-6 wk after a streptococcal pyoderma.
The severity of kidney involvement varies from asymptomatic microscopic hematuria with normal renal function to gross hematuria with acute renal failure. Depending on the severity of renal involvement, patients can develop various degrees of edema, hypertension, and oliguria. Patients are at risk for developing encephalopathy and/or heart failure secondary to hypertension or hypervolemia.
Hypertensive encephalopathy must be considered in patients with blurred vision, severe headaches, altered mental status, or new seizures. The effects of acute hypertension not only depend on the severity of hypertension but also the absolute change in comparison with the patient’s baseline blood pressure and the rate at which it has risen.
Respiratory distress, orthopnea, and cough may be symptoms of pulmonary edema and heart failure. Peripheral edema typically results from salt and water retention and is common; nephrotic syndrome develops in a minority (<5%) of childhood cases.
How to dx PSGN?
Urinalysis demonstrates red blood cells, often in association with red blood cell casts, proteinuria, and polymorphonuclear leukocyte
BLOOD UREA SERUM CREATININE
serum na,serum k, how
C3
The serum C3 level is significantly reduced in > 90% of patients in the acute phase, and returns to normal 6-8 wk after the onset. Although serum CH50 is commonly depressed, C4 is most often normal in APSGN, or only mildly depressed
Confirmation of the diagnosis requires clear evidence of a prior streptococcal infection. A positive throat culture report might support the diagnosis or might represent the carrier state. A rising antibody titer to streptococcal antigen(s) confirms a recent streptococcal infection.
The antistreptolysin O titer is commonly elevated after a pharyngeal infection but rarely increases after streptococcal skin infections. The best single antibody titer to document cutaneous streptococcal infection is the antideoxyribonuclease B level
What are the d/d?
The clinical diagnosis of poststreptococcal GN is quite likely in a child presenting with acute nephritic syndrome, evidence of recent streptococcal infection, and a low C3 level.
However, it is important to consider other diagnoses such as systemic lupus erythematosus, endo-carditis, membranoproliferative GN, and an acute exacerbation of chronic GN.
Renal biopsy should be considered only in the presence of acute renal failure, nephrotic syndrome, absence of evidence of streptococcal infection, or normal complement levels.
In addition, renal biopsy is considered when hematuria and proteinuria, diminished renal function,and/or a low C3 level persist more than 2 mo after onset. Persistent hypocomplementemia can indicate a chronic form of postinfectious GN or another disease such as membranoproliferative GN.
What are the complications?
Acute complications result from hypertension and acute renal dysfunc-tion. Hypertension is seen in 60% of patients and is associated with hypertensive encephalopathy in 10% of cases.
Other potential complications include heart failure, hyperkalemia, hyperphosphatemia, hypocalcemia, acidosis, seizures, and uremia. Acute renal failure can require treatment with dialysis.
What is the typical order for this patient?
I/o chart
Bp 6th hourly or even frequent
Daily wt
No added salt
Restrict k till urine output is better
400m/m2 +urine put as input
Diuretics
Calcium Channel blocker
Watch for seizures hyperkalemia ;breathlessness,fluid overload
Antibiotics to prevent spread of nephritogenic strains
What are the treatments for complications?
Quiz
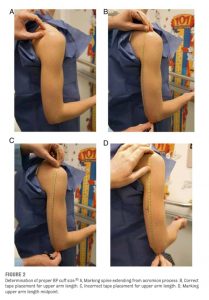
What should be breadth and length of bp cuff ?
As with older children, proper cuff size is important in obtaining accurate BP readings in neonates. The cuff bladder length should encircle 80% to 100% of the arm circumference; a cuff bladder with a width-to-arm circumference ratio of 0.45 to 0.55 is recommended
What is the cuff size for children?
How to take bp in children?
Best BP Measurement Practices
1. The child should be seated in a quiet room for 3–5 min before measurement, with the back supported and feet uncrossed on the floor.
2. BP should be measured in the right arm for consistency, for comparison with standard tables, and to avoid a falsely low reading from the left arm in the case of coarctation of the aorta. The arm should be at heart level, 90 supported, and uncovered above the cuff. The patient and observer should not speak while the measurement is being taken
.3. The correct cuff size should be used. The bladder length should be 80%–100% of the circumference of the arm, and the width should be at least 40%.
4. For an auscultatory BP, the bell of the stethoscope should be placed over the brachial artery in the antecubital fossa, and the lower end of the cuff should be 2–3 cm above the antecubital fossa. The cuff should be inflated to 20–30 mm Hg above the point at which the radial pulse disappears. Overinflation should be avoided. The cuff should be deflated at a rate of 2–3 mm Hg per second. The first (phase I Korotkoff) and last (phase V Korotkoff) audible sounds should be taken as SBP and DBP. If the Korotkoff sounds are heard to 0 mm Hg, the point at which the sound is muffled (phase IV Korotkoff) should be taken as the DBP, or the measurement repeated with less pressure applied over the brachial artery. The measurement should be read to the nearest 2 mm Hg
.5. To measure BP in the legs, the patient should be in the prone position, if possible. An appropriately sized cuff should be placed midthigh and the stethoscope placed over the popliteal artery. The SBP in the legs is usually 10%–20% higher than the brachial artery pressure.






 Superintendent, ICH.
Superintendent, ICH.