A 2-year-old male is admitted to the acute care area with tachypnea, grunting, and nasal flaring. he is hypoxic despite receiving supplemental oxygen with a high-flow nasal cannula (HFNC) at 8L/min and FiO2 0.6
He had fever, cough and breathlessness since 5days. he is also reported healtby prior to this illness.his fevr was of high grade. He had dimished appetite. He was not drowsy but had passed less urine
His immunisation is uptodate. No family members have any illness at present.no contact with TB.
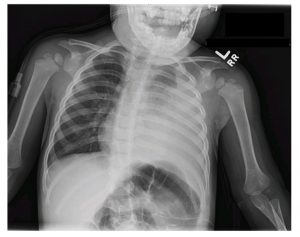
He is tachypeic, retractions + hr 170 mt, spo2 90%chest breathsounds diminished over axilla, mammary region lt, percussion dull note
What is the probable dx?
Severe Pneumonia
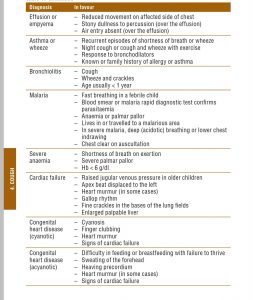
What are the d/d?
What complication is likely?
Empyema
Suspect empyema when a child with pneumonia does notvrespond usual.antibiotics in 2-4 days times
T he initial signs and symptoms are primarily those of bacterial pneumonia. Children treated with antibiotic agents may have an interval of a few days between the clinical pneumonia phase and the evidence of empyema. Most patients are febrile, develop increased work of breathing or respiratory distress, and often appear more ill
T he effusion is an empyema if bacteria are present on Gram staining, the pH is <7.20, and there are >100,000 neutrophils/µL. Cultures of the fluid must always be performed to help identify the causal organism
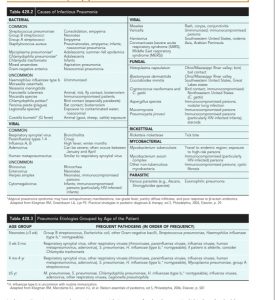
Which all agents cause pneumonia?
Nelson21
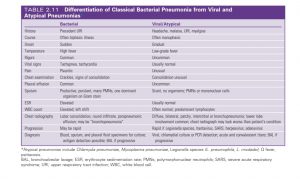
How to distinguish viral from bacterial?
How to suspect ptb?
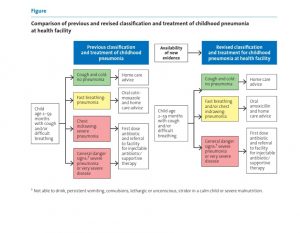
What are the national guideline for pneumonia?
Community acquired Pneumonia is categorized in to 2 types –Severe pneumonia (those with respiratory distress) and pneumonia (those with fast breathing only, treated on OPD basis).
(a) For Severe Pneumonia (Children with respiratory distress requiring indoor care)-
Under 2 months of age: o Inj Cefotaxime / Ceftriaxone and Gentamicin for 10 days
Over 2 months of age: o Inj. Ampicillin (50mg/kg/dose 6h) + Gentamicin (7.5mg/kg/day OD i.m or i.v) is used.
Inj Ampicillin can be switched to Oral Amoxycillin (45mg/kg/day TDS) once child is stable and able to take oral feeds. Total treatment duration is 7-10 days. o
In case of no response in 2 days the patient is assessed for complications like empyema, or infection at any other site.
In the absence of any complication, a 3rd generation Cephalosporin (Cefotaxime 50mg/kg/dose 6h or Ceftriaxone 75- 100mg/kg/day in two divided doses, IV ) is used and can be switched to oral Cefopodoxime (10mg/kg/day BD) once the child is able to take orally. Total treatment duration is 7-10 days.
o In case the patient has severe sepsis/ septic shock, Inj. Piperacillin + Tazobactam (90mg/kg/dose 6h) + MRSA cover with IV Vancomycin (15mg/kg/dose 6h) is recommended.
When to suspect staph pneumonia?
Rapid progression of the disease,
or Pneumatocele, or Pneumothorax, or Effusion on chest X ray
Large skin boils or abscess or infected scabies
Post measles pneumonia, which is not responding within 48 hours to the initial therapy
In severe pneumonia, use Inj.Cloxacillin or Inj Clindamycin may be added to the initial regime. OR
Oral or IV Co- Amoxyclavulanic acid can be used.
In very severe necrotizing pneumonia or for a patient in septic shock, MRSA cover should be added with IV Vancomycin Vancomycin 25-30 mg IV loading followed by 15-20 mg/kg 8-12 Hourly /)/
Teicoplanin 12 mg/kg x3 doses followed by 6 mg/kg once a day or Linezolid (10mg/kg/dose 8h).
The total duration for treatment for uncomplicated Staphylococcal pneumonia is 3-4 weeks.
How do you treat empyema?
Proper drainage : Forms the main core of treatment.
Antimicrobial Therapy: Anti- Staphylococcal penicillin (Cloxacillin 100-200 mg/kg/day) along with 3rd generation cephalosporin like Ceftriaxone may be used as first line drug.
Co-Amoxyclav is alternative first line therapy.
In seriously ill patients with disseminated staphylococcal disease and septic shock to cover for MRSA, Vancomycin is recommended. Vancomycin is less effective than the first line drugs for the commoner Methicillin sensitive strains of Staphylococcus aureus.
Children may continue to be febrile for 5-7 days after starting antibiotic therapy in the case of S. pneumoniae and H. influenzae and for 10-14 days in the case of Staphylococcus aureus.
The clinical response to therapy should be assessed with parameters such decrease in fever, normalization of lab parameters such as CBC count, CRP, decrease in drain volume, clearing in chest x-ray, improvement in the overall condition of the patient.
The decline in toxicity and fever are good signs of likely response.
In case of complete non response after 96 hours of treatment, high spiking fever and persistent drainage, second line treatment may be instituted.
Vancomycin should be substituted instead of the first line cloxacillin or co-amoxyclav.
All children with non response should be evaluated for presence of pus pockets in the pleural cavity by an ultrasound chest. Here the key lies in better drainage rather than in a change of antibiotics. Extraneous causes of fever should also be evaluated.
Why you get tachypnea and chest retractions in pneumonia?
To satisfy their oxygen needs, children who have dyspnea must increase their minute ventilation ( &VE), working harder to do so. In normal breathing, respiratory muscles work only during inspiration, and the diaphragm does most of the work. Th e work of inspiration is the sum of the work necessary to overcome the elastic forces of the lung, the tissue viscosity of the lung and chest wall, and airway resistance.
When any of these factors is increased (eg, elastic force and tissue viscosity in restrictive pulmonary disease, resistance in obstructive airway disease), the work of inspiration must increase to maintain adequate & VE.
Th e accessory muscles of inspiration (the sternocleidomastoid, anterior serratus, and external intercostal muscles) are recruited to accomplish this task. Contraction of these muscles causes forceful expansion of the thorax, resulting in an unusually large negative intrathoracic pressure. Th is negative pressure draws in the soft tissues of the chest wall and creates 1 of the classic signs of dyspnea, retractions, which may be seen in the suprasternal, infrasternal, intercostal, subcostal, and supraclavicular areas.
An alternative way to maintain an adequate &VE is to increase the rate of breathing; hence the second classic sign of dyspnea, tachypnea. Nasal f l aring and grunting are other signs during respiration.
Why you get grunting in pneumonia?
It is an effort to keep alveoli patent by increasing the end expiratory pressure by parially closing glottis early in expiration
Why nasal flaring in severe respiratory distress?
Dilator naris contracts so nasal opening is roomy reducing upper airway resistance
What is head bobbing?
The chin is lifted back during inspiration by neck muscle and falls anteriorly during expiration
Why there is subcostal retraction and prominent sternocleidomastoid in severe respiratory distress?
One of the principal functions of the thoracic wall and the diaphragm is to alter the volume of the thorax and thereby move air in and out of the lungs. During breathing, the dimensions of the thorax change in the vertical, lateral, and anteroposterior directions. Elevation and depression of the diaphragm significantly alter the vertical dimensions of the thorax. Depression results when the muscle fibers of the diaphragm contract. Elevation occurs when the diaphragm relaxes.
Changes in the anteroposterior and lateral dimensions result from elevation and depression of the ribs (. The posterior ends of the ribs articulate with the vertebral column, whereas the anterior ends of most ribs articulate with the sternum or adjacent ribs.
Because the anterior ends of the ribs are inferior to the posterior ends, when the ribs are elevated, they move the sternum upward and forward. Also, the angle between the body of the sternum and the manubrium may become slightly less acute.
When the ribs are depressed, the sternum moves downward and backward. This “pump handle” movement changes the dimensions of the thorax in the anteroposterior direction ). As well as the anterior ends of the ribs being lower than the posterior ends, the middles of the shafts tend to be lower than the two ends.
When the shafts are elevated, the middles of the shafts move laterally. This “bucket handle” movement increases the lateral dimensions of the thorax ). Any muscles attaching to the ribs can potentially move one rib relative to another and therefore act as accessory respiratory muscles. Muscles in the neck and the abdomen can fix or alter the positions of upper and lower ribs.
Subcostal retraction are due to diaphragmatic contraction. Scalene muscle can lift the ribs and sternocleido mastoid can elevate stermum and clavicle









 Superintendent, ICH.
Superintendent, ICH.
Thank you sir
Informative sir