3 year old presents with easy bruising since 3 days. He had cold 1 wk ago. He is not on medication.he has no h/o trauma.
No h/o epistaxis,hematuria,
There is no family h/o bleeding disorder.he had circumcision at 3 months of age .
He is active playful. Bruises on trunk and limbs+,no pallor ,hepatosplenomegaly
Cbc hb11gm%,wbc 12000/mm3 ,platelet 90,000
Peripheral smear normal
Dx:ITP
What is ITP?
T he most common cause of acute onset of thrombocytopenia in an otherwise well child is (autoimmune) idiopathic thrombocytopenic purpura (ITP).
1-4 wk after exposure to a common viral infection, an autoantibody directed against the platelet surface develops with resultant sudden onset of thrombocytopenia. A recent history of viral illness is described in 50–65% of children with ITP.
The peak age is 1-4 yr, although the age ranges from early in infancy to elderly. In childhood, males and females are equally affected. ITP seems to occur more often in late winter and spring after the peak season of viral respiratory illness.
How do you develop ITP?
T he exact antigenic target for most such antibodies in most cases of childhood acute ITP remains undetermined, although in chronic ITP many patients demonstrate antibodies against αIIb-β3 and GPIb. After binding of the antibody to the platelet surface, circulating antibody-coated platelets are recognized by the Fc receptor on splenic macrophages, ingested, and destroyed.
Most common viruses have been described in association with ITP, including Epstein-Barr virus and HIV . EBV-related ITP is usually of short duration and follows the course of infectious mononucleosis. HIV-associated ITP is usually chronic. In some patients, ITP appears to arise in children infected with Helicobacter pylori or rarely following vaccines.
WHAT are the clinical features?
T he classic presentation of ITP is a previously healthy 1-4 yr old child who has sudden onset of generalized petechiae and purpura. The parents often state that the child was fine yesterday and now is covered with bruises and purple dots. There may be bleeding from the gums and mucous membranes, particularly with profound thrombocytopenia (platelet count <10 × 109/L). There is a history of a preceding viral infection 1-4 wk before the onset of thrombocytopenia. Findings on physical examination are normal, other than petechiae and purpura. Splenomegaly, lymphadenopathy, bone pain, and pallor are rare. A
How do you assess severity?
A simple classification system from the United Kingdom has been proposed to characterize the severity of bleeding in ITP on the basis of symptoms and signs rather than platelet count, as follows:
1. No symptoms
2. Mild symptoms: bruising and petechiae, occasional minor epistaxis, very little interference with daily living
3. Moderate symptoms: more severe skin and mucosal lesions, more troublesome epistaxis and menorrhagia
4. Severe symptoms: bleeding episodes—menorrhagia, epistaxis, melena—requiring transfusion or hospitalization, symptoms interfering seriously with the quality of life
When should we think about alternate diagnosis?
T he presence of abnormal findings such as hepatosplenomegaly, bone or joint pain, remarkable lymphadenopathy other cytopenias, or congenital anomalies suggests other diagnoses (leukemia, syndromes). When the onset is insidious, especially in an adolescent, chronic ITP or the possibility of a systemic illness, such as systemic lupus erythematosus (SLE), is more likely.
How do you investigate?
Severe thrombocytopenia (platelet count <20 × 109/L) is common, and platelet size is normal or increased, reflective of increased platelet turnover . In acute ITP the hemoglobin value, white blood cell (WBC) count, and differential count should be normal. Hemoglobin may be decreased if there have been profuse nosebleeds (epistaxis) or menorrhagia.
Bone marrow examination is not necessary in simple ITP
Bone marrow examination shows normal granulocytic and erythrocytic series, with characteristically normal or increased numbers of megakaryocytes. Some of the megakaryocytes may appear to be immature and reflect increased platelet turnover.
Indications for bone marrow aspiration/biopsy include an abnormal WBC count or differential or unexplained anemia, as well as history and physical examination f indings suggestive of a bone marrow failure syndrome or malignancy. Other laboratory tests should be performed as indicated by the history and examination.
HIV studies should be done in at-risk populations, especially sexually active teens.
Platelet antibody testing is seldom useful in acute ITP. A direct antiglobulin test (Coombs) should be done if there is unexplained anemia, to rule out Evans syndrome (autoimmune hemolytic anemia and thrombocytopenia)
Evans syndrome may be idiopathic or an early sign of systemic lupus erythematosus, autoimmune lymphoproliferative syndrome or common variable immunodeficiency syndrome.
An ANA should be considered in adolescents, especially with other features of SLE
How do you treat?
1. No therapy other than education and counseling of the family and patient for patients with minimal, mild, and moderate symptoms, as defined earlier. This approach emphasizes the usually benign nature of ITP and avoids the therapeutic roller coaster that ensues once interventional therapy is begun. This approach is much less costly, and side effects are minimal. Observation is recommended by the American Society of Hematology guidelines for children with only mild bleeding symptoms such as bruising or petechiae.
2. Treatment with either IVIG or corticosteroids, particularly for children who present with mucocutaneous bleeding. As American Society of Hematology guidelines state, “A single dose of IVIG [intravenous immune globulin] (0.8-1.0 g/kg) or a short course of corticosteroids should be used as first-line treatment.” IVIG at a dose of 0.8-1.0 g/ kg/day for 1-2 days induces a rapid rise in platelet count (usually >20 × 109/L) in 95% of patients within 48 hr. IVIG appears to induce a response by downregulating Fc-mediated phagocytosis of antibodycoated platelets. IVIG therapy is both expensive and time-consuming to administer. Additionally, after infusion, there is a high frequency of headaches and vomiting, suggestive of IVIG-induced aseptic meningitis.
3. Corticosteroid therapy has been used for many years to treat acute and chronic ITP in adults and children. Doses of prednisone at 1-4 mg/ kg/24 hr appear to induce a more rapid rise in platelet count than in untreated patients with ITP. Corticosteroid therapy is usually continued for short course until a rise in platelet count to >20 × 109/L has been achieved to avoid the long-term side effects of corticosteroid therapy, especially growth failure, diabetes mellitus, and osteoporosis.
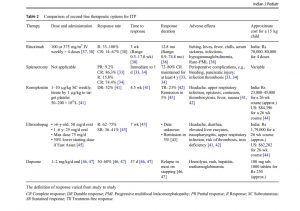
List first line drugs
List 2nd line drugs
What are the new terminologies IN ITP?
What thoughts you share with parents?
Itp is a self limiting disease
Only a few get severe bleeding especially those with mucosal bleeding
Acute itp with low counts and symptoms to be treated with first-line agents
Persistent chronicity happens in about 20%
The second line options like TPO agonists and rituximab is being increasingly used
With these agents role of splenectomy is extremely limited
Post test questions
Which is age group for ITP
5-8 Yrs
8-12 yes
1-4yrs
1-12 yes
The proposed aetiology for ITP include
Peripheral destruction of platelets
Decreased production
Megakaryocytes destruction
2 yr old with mild epistaxis and plt of 50000/mm3
No treatment
Iv ig
Steroid
Anti d
4 yr old with with hemetemesis has a plt count 8000/mm3
Start i/v fluids and iv ig
Start ffp and vitamin k
Inj methyl.prednisolone
Inj octriotide
2yr old is treated with iv ig for itp with bleeding and plt count of 5000/mm3
His plt count increases to 31000/mm3 by 1wk
Is it early response?
At one month his plt count drops to 28000/mm3
Is it initial response?
At 6 months his plt count is 25000/mm3
Is it durable response?
He is now on 10 mg steroid daily
What is it called?






 Superintendent, ICH.
Superintendent, ICH.